What are the Challenges, What are the Solutions
Implant dentistry today serves only about 5% of the patients that are eligible for implant services. That statistic alone would indicate that the dental profession is not doing an adequate job of providing dental implant services to the patient population. Implant dentistry was introduced into the market in the 1930s, but has obviously struggled to effectively capture its audience, both from a provider and patient standpoint. Unfortunately, many dental providers and patients alike are not terribly interested in this service. An argument could certainly be made that at a 5% market penetration, improvements are indicated and needed to make implant dentistry more successful and attractive. For implant dentistry to have struggled for that length of time would also indicate that it has some significant challenges. In order to effectively make a change, it is important to first identify what the challenges are and determine whether there are realistic solutions available. If not, implant dentistry will likely continue to do what it’s always done; underachieve in the marketplace.
Let’s discuss the historic challenges and offer some solutions. The implant challenges are real and have been effective in holding implant dentistry back for much too long. Solutions have arrived. The technological implant revolution is upon us. It’s exciting, it’s effective and it has a broad sweep. This revolution is significantly changing all phases of implant dentistry, including diagnostic processes, surgical protocols, and restorative approaches. The technology is quickly evolving in the dental laboratory industry with CAD technologies and fabrication of computer- generated custom titanium and ceramic abutments. This evolution is enhancing the functional and aesthetic results of clinical implant dentistry. The revolution is here but it’s not well understood. This article will also clear up some of the misunderstandings and provide help for the implant clinician to address some of those significant historic and persistent challenges.


I have addressed in prior issues of LVI Visions what I felt to be the two biggest historical challenges that implant dentistry has faced and provided workable solutions to those challenges. In summary, the two challenges were first, predictable implant placement control and second, bone loss around dental implants over time. Implant placement control challenges are completely handled by simply incorporating cone beam computerized technology (CBCT) and treatment planning software into the diagnostic and surgical protocols. In short, a CAT scan x-ray produces a three dimensional view of the area of surgical interest and the treatment planning software is used to turn that diagnostic data into a usable surgical stent. Incorporating those two tools or technologies into the diagnostic and surgical phase eliminates surgical surprise and placement position compromise. Anatomical patient limitations are discovered prior to the implant surgical event and surgical plans are modified accordingly to ensure optimum implant placement. Proper implant position or placement control with this technology is understood and achieved in the treatment phase and successfully carried over into the surgical phase.
A clinical example of poor placement control is displayed in the first two photographs. Unfortunately, in implant dentistry, this is and has been an all too common occurrence and threatens the interest and very existence of implant dentistry. With today’s technologies clinical results like this should never happen. As a comparison let’s look at a different case with a different approach.
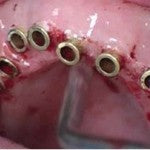
The second clinical example is in edentulous patient with a treatment objective to place 26 dental implants. The restorative plan was to have all individual crown restorations, except for a fixed implant bridge from tooth number 24 to 26. This implant case was planned using CBCT technology and treatment planning software. These photographs would certainly indicate that this case was done with significantly more control than the first case displayed. Placement control is not only predictable but absolutely achievable using this technology. Observe photographs three through eight.

3.

4.

5.
6.

7.

8.
The historic challenge of implant placement control with this technology is eliminated. This control is real and it is repeatable. There are several options in treatment planning software on the market today that provide this kind of control. Another challenge is certainly controlling the costs associated with these emerging technologies. I will discuss that in more detail later.
The second historic challenge is sustained tissue and bone health around the implant over time. Significant bone loss around dental implants over time has been a considerable challenge in implant dentistry. With today’s improved implant abutment connections and sub crestal placement protocols, bone loss around implants can be significantly reduced or eliminated with proper implant surgical and restorative protocols. Photograph nine is a clinical example of that considerable bone loss around the implant body following abutment and restoration placement. The implant abutment connection in this case is a hexed connection and the connection was not adequately accessible to the patient. In those clinical circumstances bone loss is always inevitable.


Photograph number 10 is a very similar case in terms of implant placement position. The implant abutment junction is also not reachable for the patient to maintain daily oral hygiene because of the implant placement depth, however the long-term bone health is remarkably better than the first case. The implant abutment junction in this case, is a tapered connection which is tighter and affords a much smaller microcap between the abutment and the implant. This micro gap is so small that bacteria cannot be harbored in the connection therefore bone health is sustainable over time in the sub crestal or significantly sub gingival placement protocol. A one piece implant would have some of the same clinical advantages in these cases simply because it is one piece implant abutment combination. There is no micro gap or micro movement between the implant and the abutment obviously because it is machined as a single unit. These technological advances have significantly improved bone health and bone stability around dental implants in those challenging implant cases.
Another area in implant dentistry that is quickly emerging is the dental laboratory equipment and technology. Until recently most of the implant abutments utilized were purchased by the implant manufacturers. These manufacturers produce standard or stock implant abutments or attachments for their particular implant systems. Many of these abutments once purchased were being modified or customized in the laboratory to enhance or improve functional and aesthetic characteristics of each particular implant restoration. Certainly the degree of modification is limited once the abutment is manufactured and can be self-limiting. Today in some dental laboratories the emerging technology is capable of designing and creating custom implant abutment which is used to design and create custom implant abutments in-house. These abutments are designed and manufactured specifically for each individual implant or clinical case that the laboratory restores. This technology provides much more flexibility in the restorative process. Better casecontrol with enhanced aesthetic and functional capabilities.
For example, Dental Crafters in Marshfield Wisconsin is a laboratory that is heavily engaged in the implant technology revolution. Dental Crafters uses the 3Shape dental scanner and associated Dental Design CAD software package to design custom implant abutments. This software is one of several CAD design products on the market today. The process begins by scanning a standard model from either the dentist office or from another laboratory that is outsourcing the implant abutment design and fabrication process to Dental Crafters. Ultimately this process culminates in creation of customized implant abutment milled from either titanium or zirconium. The design process is broken down into several scanning steps as well as the actual designing of the abutment. The major steps are summarized below.


The CAD technician scans the model with the scanning abutment pin in place. The scanning abutment pin is a metal or plastic alignment pin that when scanned represents the placement of the implant in the mouth. Because each implant system is different, a proprietary scanning abutment pin is specifically designed for each implant system. The laboratory purchases these alignment pins from the implant manufacturers. The orange cylinder in the photograph represents the proprietary scan abutment pin for this case, which gives the software the proper orientation of the implant and its connection to the abutment. This scan also allows the scanner to capture the interproximal areas between the teeth as well as the tissue around the abutment site.
Photograph 13 is a representation of a scanning abutment prior to any custom design of the implant abutment. Photograph 14 is a proposed abutment that could be milled out of the titanium or zirconium scanning abutment. Photograph 15 is a custom abutment design in relation to the surrounding teeth. The CAD technician can utilize many design and measurement tools to fully design, customize and mill a titanium or zirconium abutment. An additional scan is taken by the CAD technician of the antagonist arch which will be used to determine the clearance for the restoration between the upper and lower arches.

13.

14.

15.
This technology is a game changer in the laboratory. The laboratory can design a custom abutment to maximize proper orientation, build a proper abutment profile coming out of the tissue, and place finish lines for the crown margin at the appropriate tissue heights. Each of those characteristics alone is of significant importance in restorative implant aesthetics. Having the ability to control all of those characteristics in the design process for each case is a dramatic improvement from where the laboratory capabilities were a very short time ago. I suspect the whole restorative implant market will change quickly with this technology. Fully customizable laboratory fabricated implant abutments will soon be the standard and stock implant abutments will be a thing of the past. Why wouldn’t the implant and laboratory industry embrace this technology? The answer is that they will simply because it is profoundly better than what they’re accustomed to. This technology provides a much simpler solution for the challenging cases that dental laboratories often receive from their doctor’s offices.


A similar technique being used in laboratories today is purchasing only the titanium connection to the implant from the manufacturing source and then using CAD software to construct a zirconium core which is looted to the titanium abutment connection. A zirconium crown then is fabricated and looted to the zirconium core. The distinct clinical advantage in this approach is that the implant abutment connection is titanium and has the strength of titanium. However, the remaining portion of the abutment is zirconium and has the cosmetic advantage of a zirconium abutment coming through the tissue to support the restoration. In other words these cases have a strong titanium connection that is much less likely to fracture than a ceramic abutment while retaining the aesthetic advantages of a ceramic abutment. It’s really the best of both worlds in the restorative process which makes it one of my favorite implant abutment choices.
I would suspect at this point in the article you are intrigued by the technological advances and certainly understand their usefulness in solving some of implant dentistry’s significant challenges. The 800 pound gorilla that remains in the room is: what is the cost of this technology, and is it realistic and affordable? I have incorporated all of these technologies into my implant practice and find them very useful and affordable. To help you better understand the economic considerations in the use of this technology I will share my implant fee schedule as well as the real costs associated with those implant services and the technology utilized. In order to make the numbers realistic I will assume most doctors will rent the CT images needed to do a proper diagnosis. I own a CT machine in the office so my numbers would be slightly different on the revenue side versus expense side but for the sake of this exercise I will assume the images are rented from an outside source.
Granted these are my expenses and my revenues from my office and they may vary dramatically in your particular office environment. Your revenues may be significantly higher or lower based on your practice model. I did not include in this comparison additional cost such as practice overhead, initial equipment investment or fixed practice costs. I also did not include other revenue potential that implant dentistry provides to the practice. It is strictly meant as a guideline to the fixed costs associated with guided implant surgery and custom implant abutments and the restoration process.


It is also understood based on analysis above that this technology is affordable even in the worst-case financial scenario, which is a single implant placement and restoration case. The cost of the technology becomes negligible and considerably more favorable in implant cases involving multiple implants.
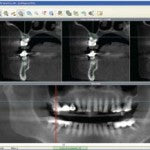
Photographs 20 through 26 are a clinical example of a four tooth im-plant case using all the latest technologies. This clinical example is a patient 85 years of age with some medical compromise. Treatment plan is to extract tooth numbers 3, 5 and 12. Both three and five have apical abscesses and a poor prognosis. Tooth number 12 has a root fracture and a hopeless prognosis. CT technology and treatment planning software were used to plan and place four dental implants in the most ideal position. Immediate extraction and sub crestal placement of the implants were done to expedient the treatment process as well as maintain adequate crestal bone health. Tissue and bone health are apparent on the clinical photographs shown. After four months of healing, impressions were taken and Dental Crafters used its CAD design software to make custom abutments. These abutments had a titanium implant abutment connection or junction with a zirconium abutment core and crown. All of these technologies combined guarantee proper implant placement position and enhanced function and aesthetics of the restorations. 21st century implant dentistry guarantees better control, better function and aesthetics.
20.

21.

22.

23.

24.

25.
In summary, implant dentistry and its processes are changing quickly. These technological advancements are improving diagnostic, surgical, and restorative protocols. These improvements provide better control of implant cases and guarantee a more functional and aesthetic outcome for our patients. These improvements solve many of our historic implant challenges and make implant dentistry more attractive to our profession and to the patients that we serve. The technology is effective and fortunately for all of us, providers and patients alike, it is here to stay. I would encourage every dental practitioner to get involved in implant dentistry.


